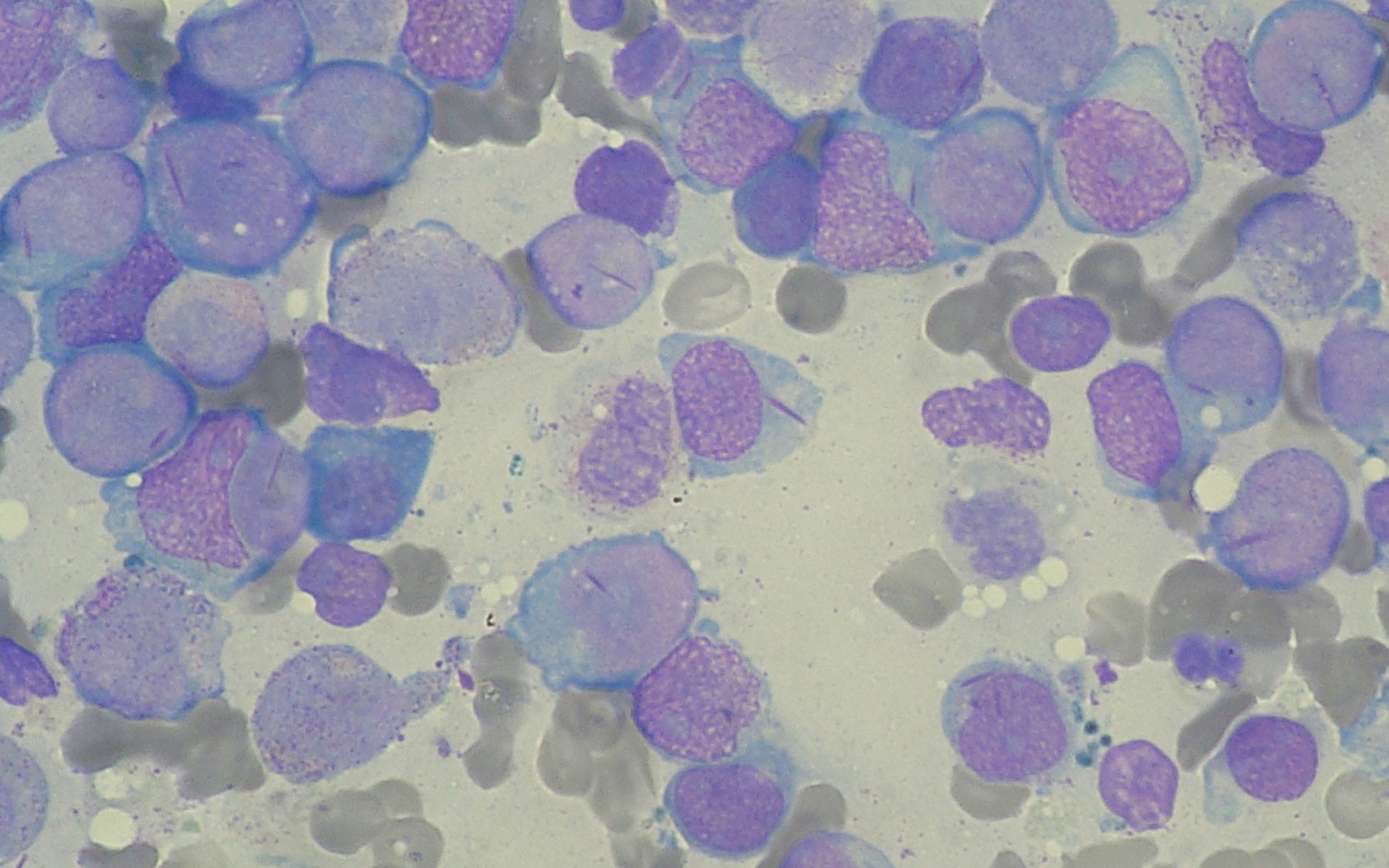
Knowing how the drug, called JQ1, disturbs gene expression could help improve the drug and reveal additional targets
Cold Spring Harbor, NY — Inhibiting a protein called BRD4 critical to the survival of acute myeloid leukemia (AML) cells has shown to be an effective therapeutic strategy. But the mechanism that explains how the protein works has remained a mystery. Now, scientists at Cold Spring Harbor Laboratory (CSHL) have discovered the larger cancer-causing pathway that the protein fits into.
The discovery points to additional molecular targets for the development of drugs to treat AML as well as other cancers. The results appear online today in Molecular Cell.
In 2011, CSHL Associate Professor Christopher Vakoc and colleagues identified potential drug targets for AML—a relatively rare blood cell cancer—using a technology called RNA interference, in which RNA molecules are mobilized to inhibit gene expression. “We systematically went hunting for things required by leukemia cells to grow and thrive,” says Vakoc.
Out of that approach came BRD4. By reading certain epigenetic marks, or chemical tags, attached to chromatin—the combined package of DNA and proteins around which the genetic material is coiled within the cell nucleus—BRD4 helps control the pattern of which genes are switched on. Leukemia cells were found to be extremely sensitive to changes in the BRD4 protein. In a bit of serendipity, drugs to inhibit BRD4 had just been developed for other purposes. Vakoc and his colleagues tested these drugs and found that one in particular, called JQ1, worked well against a mouse model of the most aggressive form of AML.
In the past few years, several groups have reported similar therapeutic results in mice using JQ1 and closely related drugs. “It’s been very satisfying to see that other research laboratories have independently validated BRD4 inhibition as an effective therapeutic approach in leukemia-bearing mice,” says Vakoc.
Due to the overwhelming evidence of their effectiveness in mice, inhibitors of BRD4 moved into clinical trials starting in 2013. Currently, there are 12 clinical trials targeting BRD4 in leukemia and other cancers. Last year, clinical trial findings presented at the AACR cancer meeting indicated that an oral inhibitor of BRD4 similar to JQ1 had led to complete remissions in leukemia patients.
“Once we published our first BRD4 paper in 2011, the main objective in our lab has been to understand why these drugs work,” says Vakoc. “Knowing the mechanism of action of a drug is essential to making the drug better because there will likely be many generations of BRD4 inhibitors with improved performance.”
In the current study, the team of scientists in the Vakoc lab, led by post-doctoral fellow Jae-Seok Roe, discovered that BRD4 works very closely with an ensemble of proteins called transcription factors that also bind to DNA and very selectively control the activity of certain genes. The transcription factors that BRD4 associates with control blood formation and essentially give blood cells their identity. In leukemia, which Vakoc calls a disorder of mistaken blood identity, blood cells undergo genetic changes that prevent stem cells from maturing into white blood cells. “The leukemia cells try to be immortal by staying in stem cell state forever,” says Vakoc.
The result is leukemia: an accumulation of immature cells with no useful function that crowd out viable blood cells in bone marrow, thereby decreasing the ability to fight infection and the ability to form blood clots in response to injury. Anemia eventually develops because the blood cannot sufficiently supply the body with oxygen.
The team had originally discovered in 2011 that the drug JQ1 can make leukemia cells shed their leukemia characteristics and mature, or differentiate, into normal appearing white blood cells.
In the current study, the researchers also identified an intermediary molecule called p300, which also works closely with BRD4 and the leukemia-associated transcription factors. Active areas of research in Vakoc’s lab include exploring other players in the pathway, particularly the molecules that BRD4 controls, and learning more about the transcription factors. “This new work is leading us to realize how important transcription factors are for the immortality of these leukemia cells,” Vakoc says. “Clearly they are driving the aggressive behavior of the disease, but can be blocked by JQ1.”
In a related study from the Vakoc lab that was published April 25 in eLife, the team identified a way to target a protein called TRIM33 as a means of modulating the actions of a transcription factor called PU.1 in B-cell lymphoblastic leukemia, a cancer of the white blood cells that make antibodies. Although parallels exist between the activity of BRD4 and TRIM33, a major difference lies in the specificity of the proteins. TRIM33 functions with a single transcription factor at a single binding site near the Bim gene. In contrast, BRD4 is associated with many transcription factors at many binding sites throughout the genome.
“Our work raises a provocative question,” says Vakoc. “What if we target transcription factors directly? Would our therapies be more effective if we went to the source of gene expression control?”
Directly targeting transcription factors could be much more effective than chemotherapy or even JQ1, he speculates. Chemotherapy makes all growing cells sick—cancer cells, but also cells in the gut, skin, and blood, among others. “There’s no specificity as to which tissues are affected,” says Vakoc. “Transcription factor targeting, on the other hand, would potentially zero in on one type of tissue.”
Written by: Chris Palmer, Science Writer | publicaffairs@cshl.edu | 516-367-8455
Funding
The research described in the release was supported by the NIH, Alex’s Lemonade Stand Foundation, the V Foundation, the Martin Sass Foundation, the Lauri Strauss Leukemia Foundation, Burroughs Wellcome Fund, Japan Society for the Promotion of Science, and Boehringer Ingelheim Fonds.
Citation
“BET bromodomain inhibition suppresses the function of hematopoietic transcription factors in acute myeloid leukemia,” appears online May 14, 2015 in Molecular Cell. The authors are Jae-Seok Roe, Fatih Mercan, Keith Rivera, Darryl J. Pappin, and Christopher R. Vakoc. The paper can be viewed at: http://www.sciencedirect.com/science/journal/10972765
“The transcriptional cofactor TRIM33 prevents apoptosis in B lymphoblastic leukemia by deactivating a single enhancer,” appeared online April 25, 2015 in eLife. The authors are Eric Wang, Shinpei Kawaoka, Jae-Seok Roe, Junwei Shi, Anja F. Hohmann, Yali Xu, Anand S. Bhagwat, Yutaka Suzuki, Justin B. Kinney, Christopher R. Vakoc. The paper can be viewed at: http://elifesciences.org/
Principal Investigator

Chris Vakoc
Professor
Alan and Edith Seligson Professor of Cancer Research
Cancer Center Deputy Director of Research
M.D., Ph.D., University of Pennsylvania, 2007