A region of the brain called the amygdala is responsible for powerful emotions like fear. Now, researchers have found the amygdala may also be to blame for overeating. Cold Spring Harbor Laboratory (CSHL) Professor Bo Li has discovered a group of neurons in the amygdala that drives mice to eat fatty or sugary foods—even when they’re not hungry. Therapeutics targeting these neurons could lead to new treatments for obesity with minimal side effects.
Like most people, mice also tend to find foods high in fat and sugar the tastiest. They may indulge in these treats for pleasure, rather than for survival. The neurons Li and his colleagues studied trigger this behavior, called hedonic eating. Li notes:
“Even if the animal is supposed to stop eating because they are already full, if those neurons are still active, it can still drive those animals to eat more.”
Almost no one succeeds in long-term weight management when treating obesity, Li says. Metabolic processes in the body often reverse any progress that’s made. Therapeutics can help increase the odds of successful treatment, but many drugs have unwanted side effects. “The medications currently available to aid weight management can cause significant side effects. So, a more targeted approach is needed,” Li says. “Identifying the brain circuitry that controls eating is important for developing better treatment options for people who struggle to control their weight.”
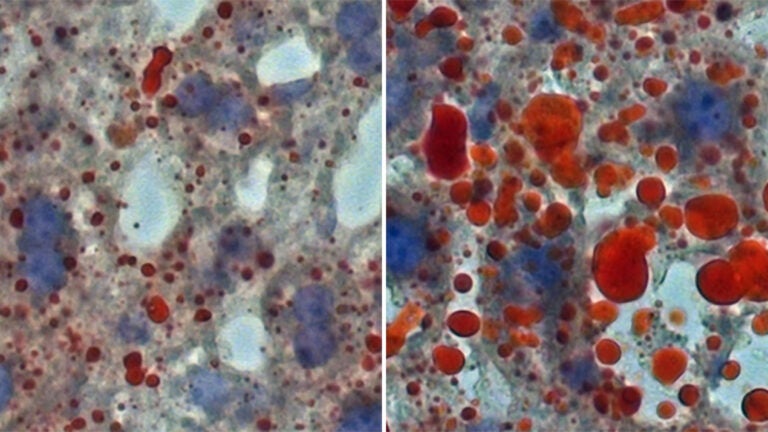
When the team switched off the specific neurons, mice weren’t drawn to the fatty, sugary foods that had tempted them before. “They just happily ate and stayed healthy,” Li says. “They not only stopped gaining weight, but also seemed to be much healthier overall.” Switching these neurons off reduced overeating and protected against obesity. It also boosted the animals’ physical activity, leading to weight loss and better metabolic health.
Li and his team are exploring ways to manipulate the neurons that trigger hedonic eating. The next step, he says, is to map out how these neurons respond to different types of food and see what makes them so sensitive. He hopes this collaboration will lead to new strategies for effective anti-obesity therapeutics.
For this study, Li and CSHL Associate Professor Stephen Shea combined their neuroscience expertise with CSHL Assistant Professor Semir Beyaz’s expertise in gut and nutrition research. They also collaborated with CSHL Assistant Professor Tobias Janowitz, an expert in metabolism and endocrinology. It’s part of an ongoing, multidisciplinary initiative at CSHL to research the connections between the brain and the body.
Written by: Jennifer Michalowski, Science Writer | publicaffairs@cshl.edu | 516-367-8455
Funding
European Molecular Biology Organization, Swedish Research Council, the Charles H. Revson Senior Fellowship in Biomedical Science, the National Institutes of Health, Cold Spring Harbor Laboratory and Northwell Health Affiliation, Feil Family Neuroscience Endowment, German Academic Scholarship Foundation
Citation
Furlan, A., et al., “Neurotensin neurons in the extended amygdala control dietary choice and energy homeostasis”, Nature Neuroscience, October 20, 2022. DOI: 10.1038/s41593-022-01178-3
Principal Investigator

Bo Li
Professor
Robert Lourie Professor of Neuroscience
Ph.D., The University of British Columbia, 2003