Imagine you wake up in a hospital without a single memory of the last month. Doctors say you had a series of violent episodes and paranoid delusions. You’d become convinced you were suffering from bipolar disorder. Then, after a special test, a neurologist diagnoses you with a rare autoimmune disease called anti-NMDAR encephalitis. This is what happened to Susannah Cahalan, a New York Post reporter who would go on to write the best-selling memoir Brain on Fire: My Month of Madness.
Anti-NMDAR encephalitis can lead to hallucinations, blackouts, and psychosis, says Cold Spring Harbor Laboratory Professor Hiro Furukawa. It mostly affects women ages 25 to 35—the same age at which schizophrenia often presents itself. But what’s happening in anti-NMDAR encephalitis is something else.
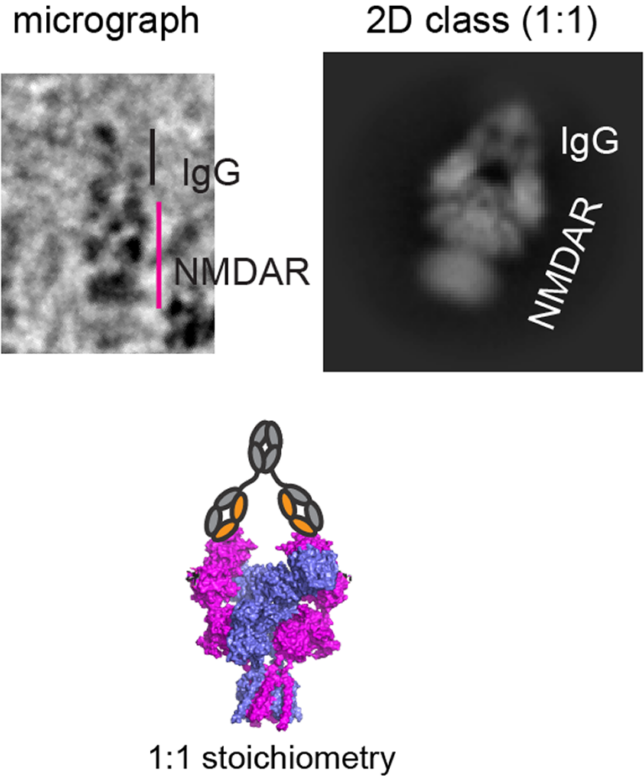
Furukawa specializes in NMDARs, brain receptors that play a critical role in cognition and memory. “In anti-NMDAR encephalitis, antibodies bind to those receptors and prevent them from working,” he explains. As an autoimmune response, the brain becomes inflamed—hence, Brain on Fire.
While some treatments are available, their effectiveness varies depending on symptom severity. New research from the Furukawa lab may explain why. In a recent study, Furukawa and colleagues map how antibodies from three patients bind to NMDARs. They find that the way in which each of the three antibodies binds to NMDARs differs. The discovery marks an important step in gaining a fuller understanding of anti-NMDAR encephalitis, a condition first diagnosed in 2008. Furthermore, it suggests personalized medicine may be critical for treating this disease.
“Distinct binding patterns manifest in different functional regulation levels in NMDARs,” Furukawa explains. “This affects neuronal activities. So, different binding sites may correspond to variations in patients’ symptoms.” Uncovering those correlations could lead to more precise therapeutic strategies. Imagine, for example, that scientists identify several binding sites common among encephalitis patients. Pharmacologists could then design new drugs to target these sites. But that’s not all. Personalized medicine could also mean more accurate diagnoses, Furukawa says.
“It’s still a rare disease, but it could be misdiagnosed or underdiagnosed. Therefore, we need to spread awareness. Could, for example, some schizophrenic patients have this disease? Could it be caused by antibodies?”
Currently, it’s said that anti-NMDAR encephalitis affects one in 1.5 million people. Yet, in time, we may find it’s more common than previously assumed. That’s a scary thought. However, it could explain why existing psychiatric medicine does not work for some people diagnosed with bipolar disorder and other mental health conditions—a huge revelation for patients as well as the families and therapists who care for them.
Written by: Jen A. Miller | publicaffairs@cshl.edu | 516-367-8455
Funding
National Institutes of Health, Austin’s Purpose, Robertson Research Fund, Doug Fox Alzheimer’s Fund, Heartfelt Wings Foundation, Gertrude and Louis Feil Family Trust, German Research Foundation, German Federal Ministry of Education and Research, Schilling Foundation
Citation
Michalski, K., et al., “Structural and functional mechanisms of anti-NMDAR autoimmune encephalitis”, Nature Structural & Molecular Biology, September 3, 2024. DOI: 10.1038/s41594-024-01386-4
Jain, A., et al., “Dendritic, delayed, stochastic CaMKII activation in behavioural time scale plasticity”, Nature, October 9, 2024. DOI: 10.1038/s41586-024-08021-8
Core Facilites
Principal Investigator

Hiro Furukawa
Professor
Cancer Center Member
Ph.D., The University of Tokyo, 2001

