For the first time since the coronavirus disease 2019 (COVID-19) outbreak appeared in the United States new research from the Feinstein Institutes for Medical Research provides a comprehensive analysis of the New York population that sought care from Northwell Health, New York State’s largest health system.
The study, published July 8 in the journal Clinical Infectious Diseases, leveraged the high degree of technical and data standardization of Northwell Health Laboratories to analyze 46,793 patients who were tested for the virus between March 8 and April 10, 2020. Of those tested, 26,735 or 57.1% of patients revealed a positive diagnosis. About 30% of those who tested positive for COVID-19 (8,174 people) were hospitalized.
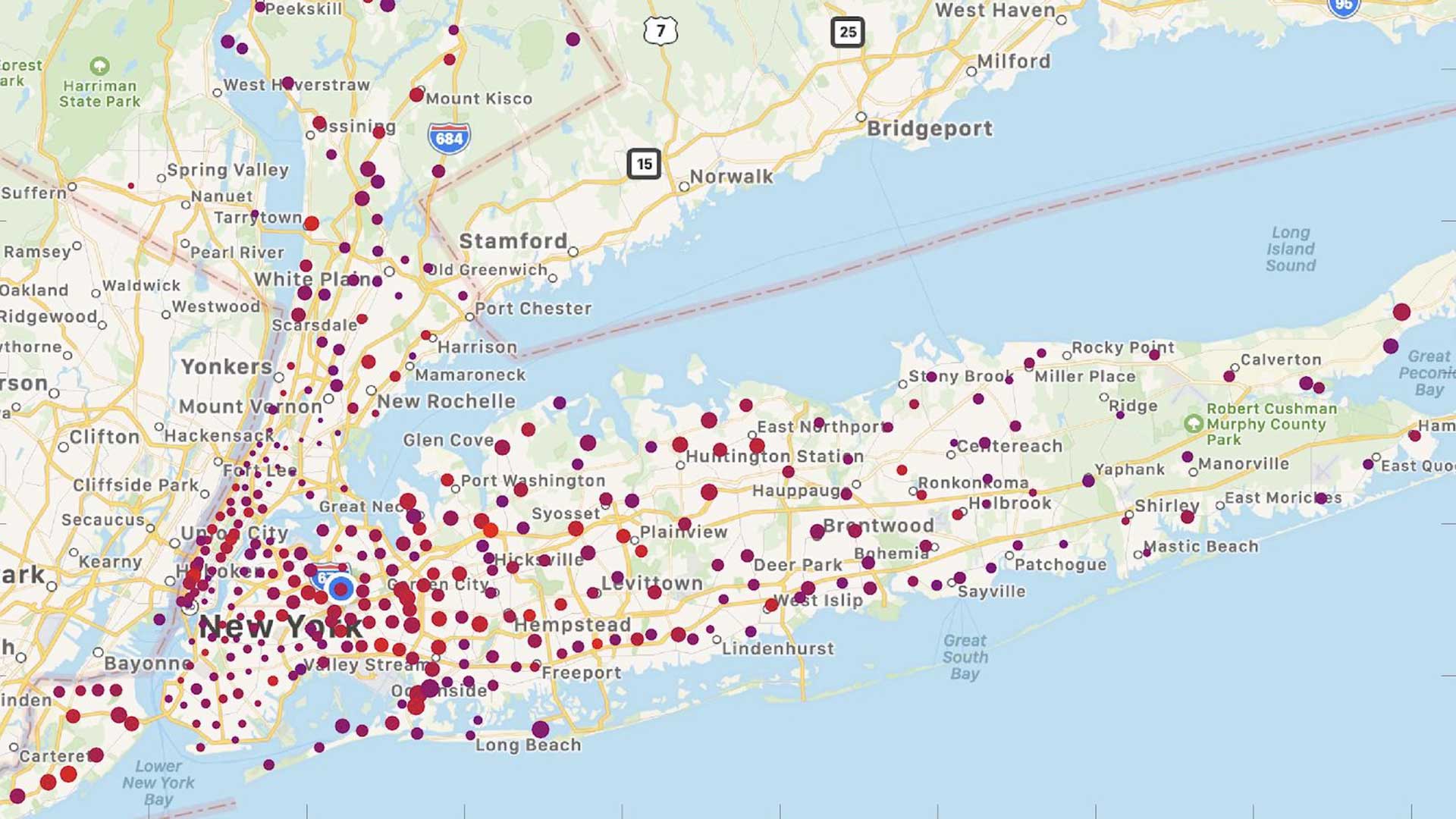
This study provides further evidence that COVID-19 infection was widespread across the greater New York metropolitan area at the time that diagnostic testing became available in early March, and provides detailed demographic and geographic information about persons who were tested during the first five weeks of the outbreak. According to Cold Spring Harbor Laboratory (CSHL) Professor Partha Mitra, who was an author on the study:
A striking observation is the remarkable degree of spatial heterogeneity—even neighboring zip codes showed very different per capita numbers of cases, and the growth patterns in time also differed widely. Understanding this heterogeneity better may be important in developing effective control strategies.”
Partha Mitra
The highest positive cases were noted in Queens County (68.5% of persons tested), Kings County (62.3%), and Bronx County (59.2%). The lowest positive rates were noted for Westchester County (46.4%) and Suffolk County (51.2%).
“To better understand how COVID-19 spreads, we need to know where people who got infected by the virus lived, when they got infected, and then learn as much about them as we can,” said James Crawford, M.D., Ph.D., professor at the Feinstein Institutes and senior author of the paper. “This information helps us better understand who is at risk of getting COVID-19 and can help inform other regions that are still on the upswing of viral spread. This study also will help us prepare for future surges of this or other viruses.”
The researchers found that males were more likely to be positive for COVID-19 than females, and test positivity rates increased progressively with age. For both males and females age 25 and under, the estimated regional case incidence by April 10 was well below 1%. For females age 25 and above, the estimated regional case incidence rose steadily from 1.7% to 2.6% through age 84 and was 4.7% for age 85 and above. For males age 25 and above, estimated regional case incidence rose from 1.6% at age 25 to 4.4% through age 84 and was 6.0% for age 85 and above.
Northwell’s service area includes some of the most diverse neighborhoods in the world. In regard to race, the Black population (both sexes) registered a positivity rate of 67.8% compared with the Asian population (62.3%) and White population (55.5%). Information was not available for test positivity rates in the Hispanic population. The highest test positivity rates were among Black males (72.1%) and Asian males (71.6%).
Mitra points out, “COVID-19 was likely prevalent in the NYC/Long Island area by the time testing began in early March. This data set is fairly unique in providing a snapshot into the early growth of the case numbers with zip-code level granularity. The other data available from these early times are county-based.”
The majority of hospital admissions for COVID-19 (7,292 persons) were immediately upon presentation of a symptomatic patient to a hospital emergency room. However, a small number of persons who tested positive for COVID-19 as outpatients were subsequently admitted to the hospital (882 persons), a median of five days after their test had been performed.
“After treating more than 50,000 COVID-19 patients, 1,500 of whom were enrolled in clinical trials, our data is a powerful weapon against the virus,” said Kevin Tracey, M.D., president and CEO of the Feinstein Institutes. “Dr. Crawford’s research is a key part of that effort and will help us understand the evolution of the COVID-19 pandemic.”
This research was done in collaboration between The Feinstein Institutes for Medical Research and CSHL.
Funding
National Institute on Aging of the National Institutes of Health and the National Library of Medicine of the National Institutes of Health
Citation
Reichberg, S.B., et. al., “Rapid Emergence of SARS-CoV-2 in the Greater New York Metropolitan Area: Geolocation, Demographics, Positivity Rates, and Hospitalization for 46,793 Persons Tested by Northwell Health,” Clinical Infectious Diseases, July 8, 2020 DOI: 10.1093/cid/ciaa922
About the Feinstein Institutes
The Feinstein Institutes for Medical Research is the research arm of Northwell Health, the largest health care provider and private employer in New York State. Home to 50 research labs, 3,000 clinical research studies and 5,000 researchers and staff, the Feinstein Institutes raises the standard of medical innovation through its five institutes of behavioral science, bioelectronic medicine, cancer, health innovations and outcomes, and molecular medicine. We make breakthroughs in genetics, oncology, brain research, mental health, autoimmunity, and are the global scientific leader in bioelectronic medicine—a new field of science that has the potential to revolutionize medicine. For more information about how we produce knowledge to cure disease, visit http://feinstein.northwell.edu and follow us on LinkedIn.